Possible link between cell membrane viscosity, nerve cell membrane intergrity and nerve-muscle control Jan 3rd 2017
( This line of thought started while I was binging on Netflix, specifically, season 1 episode 4 & 5 of "The Deep" )
There might be a link between cell membrane viscosity, nerve cell membrane integrity and nerve-muscle control.
http://oceanservice.noaa.gov/facts/pressure.html
According to the National Ocean Service website, the pressure increases by 1 atmosphere every 10 meters. So at 1000 meters, the pressure is 100 atmospheres, or 100 times the pressure at sea level.
http://www.ftexploring.com/askdrg/askdrgalapagos2.html
Sperm whales hand have been documented to go up to 1.6 miles deep.
http://discovermagazine.com/2001/aug/featphysics
This 2001 august article in Discover Magazine lists some adaptations to the crushing pressures at the ocean depths of deep sea diving animals that dive up to 1 mile deep. These deep sea divers include Weddell seals and elephant seals that have these adaptations:
1) Lungs are collapsed completely
2) Oxygen is stored mostly in their muscles during a deep dive (i.e. in myoglobin)
3) the cell membrane is more fluid (more unsaturated fats instead of saturated fats)
https://www.breatheology.com/articles/mammalian-dive-response/
What the previous article doesn't mention that humans can do is covered in this website:
1) Bradycardia (slowing of heart rate)
2) Peripheral vasoconstriction (blood is shunted away from exterior limbs)
3) Blood shift fills chest cavity with plasma (so the lungs aren't crushed, plasma later reabsorbed)
4) Windpipe closes to prevent lungs from filling with water (infants to 6 months old only)
This effect occurs in humans as soon as the face comes into contact with cold water.
However, the effect in human beings is puzzling as instead of shunting blood away from the limbs like diving mammals, the human circulatory system supplies the limbs with even more blood to keep them warm, thus losing heat even quicker.
(The mammalian diving response is explained in this physiological paper with extensive citations here: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3768097/ ) One line in particular stood out to me, " Is it [Diving Reflex] the “master switch of life” (216)? "
(Central Control of breathing in mammals: neuronal circulatory, membrane properties and neural transmitters : https://www.ncbi.nlm.nih.gov/pubmed/7831394/ )
(The correlation in membrane properties is explored in this paper : http://www.nrcresearchpress.com/doi/abs/10.1139/z01-047?journalCode=cjz#.WGwfXtTzIVQ )
(While the peculiarities of deep sea black fish in phospholipid membrane and fatty acid composition studied here http://link.springer.com/article/10.1134%2FS0022093012010069 originally published in Russian)
while this link explains why the black sea is a unique place to study marine life http://blacksea-education.ru/blacksea.shtml
How is this related to nerve-muscle disorders such as Parkinson's and ALS you ask?
The nervous system might be dysfunctional due to (and this is entirely hypothetical) the nerves being too rigid (too much saturated) or too fluid (too much poly-unsaturated fats). Whether it is genetic or environmental (or both, gene-environment interactions), the solution could be postulated to be temperature to treat.
The precise details for such a treatment is described here;
http://www.mayoclinic.org/tests-procedures/hyperbaric-oxygen-therapy/basics/definition/prc-20019167
But what if we included temperature along with pressure in the nerve treatment? (along with an oral neuro-chemical treatment I suppose, but I don't have data to support a neurochemical-temperature-pressure controlled treatment, and I have a reluctance to include a chemical fix if a temperature and pressure treatment might work.
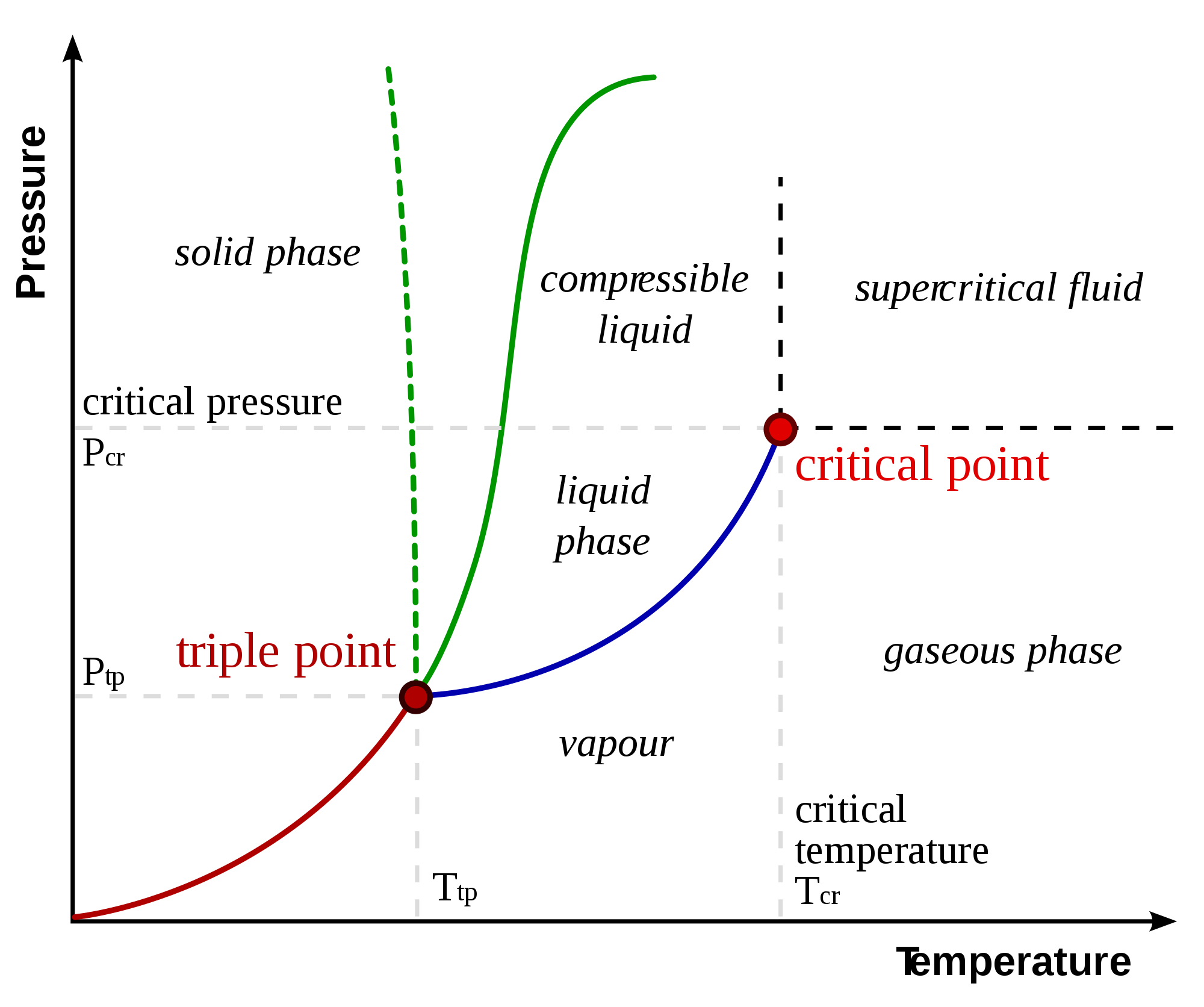
Assuming the phospholipids are too fluid, the patient could be put in a hyperbaric chamber with a higher atmospheric pressure. Whether this would affect the myelin sheath would take a longer period of time in the hyperbaric chamber to determine (3-4 days maybe?). However, it would be ill-informed to place the patience in a hyperbaric chamber without an electric blanket, to raise the body temperature at the same time while raising the pressure per this critical point graph.
The danger would be in case the boiling point of blood plasma might be reached too quickly in the higher pressure (The same reason why it is hard to boil water at high altitudes with low pressure).
One other thing, having the fatty tissues behave differently at a higher pressure may affect how how a phospholipid membrane behaves towards serotonin and dopamine in neurochemical cell signaling.
Both ALS and Parkinson's disease have age related although the disease can appear at any age, it usually shows up after 20 and have a higher rate of occurrence after 50 to 60 years of age.
Could a person's ability to digest, absorb and/or repair fatty tissue slow down or become dysfunctional in relation to age? I guess it's like a 3 legged tripod stand, should any one of the legs in the tripod for healthy lipid-based membranes fail (digestion, absorption or repair) the entire system of having healthy fatty tissue might fail, unless there was some fail safe ability for humans to convert sugar to fat in humans.
Perhaps one treatment would be to exercise, which could raise the body's core temperature and temporarily restore the functionality of nerve tissue, (cycling helping patients with Parkinson's disease, a news story that broke in 2010)
http://www.medicalnewstoday.com/articles/253197.php
http://www.nytimes.com/2010/04/01/health/01parkinsons.html
http://www.foxnews.com/health/2012/04/24/bike-riding-helps-parkinsons-patients-ease-their-symptoms.html
So to reiterate, could Parkinson's disease (along with the main symptom of autonomous nervous system dysfunction) also be correlated with loss of thermoregulation?
Incidentally, another fatty tissue shows age correlation: the skin.
According to this website, 90% of people have age related sun spots by the time they are 60. This is something we can see all around us, people over 50 tend to have sun spots, and people close to 70 have a lot of large sun spots. https://zoskinhealth.com/blog/out-of-the-dark-reversing-sun-spots/
(and maybe there might be an entirely differently chemical co-factor I'm missing that is affecting phospholipid membrane permeability that is also age related).
I think that in studying the skin's sun spots (which thanks for the beauty industry, we have a lot of data on) it may be cheaper and quicker to draw parallels as to how rates of ALS and Parkinson's risk rate show up in relation to age as they are both fatty tissue type dysfunctions.
Oh dear I'm gradually turning into a theoretically biologist, as opposed to a real biologist.
found this later on
https://www.reddit.com/r/askscience/comments/1vfliv/how_do_deepsea_fishes_not_get_crushed_by_the/
There might be a link between cell membrane viscosity, nerve cell membrane integrity and nerve-muscle control.
http://oceanservice.noaa.gov/facts/pressure.html
According to the National Ocean Service website, the pressure increases by 1 atmosphere every 10 meters. So at 1000 meters, the pressure is 100 atmospheres, or 100 times the pressure at sea level.
http://www.ftexploring.com/askdrg/askdrgalapagos2.html
Sperm whales hand have been documented to go up to 1.6 miles deep.
http://discovermagazine.com/2001/aug/featphysics
This 2001 august article in Discover Magazine lists some adaptations to the crushing pressures at the ocean depths of deep sea diving animals that dive up to 1 mile deep. These deep sea divers include Weddell seals and elephant seals that have these adaptations:
1) Lungs are collapsed completely
2) Oxygen is stored mostly in their muscles during a deep dive (i.e. in myoglobin)
3) the cell membrane is more fluid (more unsaturated fats instead of saturated fats)
https://www.breatheology.com/articles/mammalian-dive-response/
What the previous article doesn't mention that humans can do is covered in this website:
1) Bradycardia (slowing of heart rate)
2) Peripheral vasoconstriction (blood is shunted away from exterior limbs)
3) Blood shift fills chest cavity with plasma (so the lungs aren't crushed, plasma later reabsorbed)
4) Windpipe closes to prevent lungs from filling with water (infants to 6 months old only)
This effect occurs in humans as soon as the face comes into contact with cold water.
However, the effect in human beings is puzzling as instead of shunting blood away from the limbs like diving mammals, the human circulatory system supplies the limbs with even more blood to keep them warm, thus losing heat even quicker.
(The mammalian diving response is explained in this physiological paper with extensive citations here: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3768097/ ) One line in particular stood out to me, " Is it [Diving Reflex] the “master switch of life” (216)? "
(Central Control of breathing in mammals: neuronal circulatory, membrane properties and neural transmitters : https://www.ncbi.nlm.nih.gov/pubmed/7831394/ )
(The correlation in membrane properties is explored in this paper : http://www.nrcresearchpress.com/doi/abs/10.1139/z01-047?journalCode=cjz#.WGwfXtTzIVQ )
(While the peculiarities of deep sea black fish in phospholipid membrane and fatty acid composition studied here http://link.springer.com/article/10.1134%2FS0022093012010069 originally published in Russian)
while this link explains why the black sea is a unique place to study marine life http://blacksea-education.ru/blacksea.shtml
How is this related to nerve-muscle disorders such as Parkinson's and ALS you ask?
The nervous system might be dysfunctional due to (and this is entirely hypothetical) the nerves being too rigid (too much saturated) or too fluid (too much poly-unsaturated fats). Whether it is genetic or environmental (or both, gene-environment interactions), the solution could be postulated to be temperature to treat.
The precise details for such a treatment is described here;
http://www.mayoclinic.org/tests-procedures/hyperbaric-oxygen-therapy/basics/definition/prc-20019167
But what if we included temperature along with pressure in the nerve treatment? (along with an oral neuro-chemical treatment I suppose, but I don't have data to support a neurochemical-temperature-pressure controlled treatment, and I have a reluctance to include a chemical fix if a temperature and pressure treatment might work.
Assuming the phospholipids are too fluid, the patient could be put in a hyperbaric chamber with a higher atmospheric pressure. Whether this would affect the myelin sheath would take a longer period of time in the hyperbaric chamber to determine (3-4 days maybe?). However, it would be ill-informed to place the patience in a hyperbaric chamber without an electric blanket, to raise the body temperature at the same time while raising the pressure per this critical point graph.
The danger would be in case the boiling point of blood plasma might be reached too quickly in the higher pressure (The same reason why it is hard to boil water at high altitudes with low pressure).

One other thing, having the fatty tissues behave differently at a higher pressure may affect how how a phospholipid membrane behaves towards serotonin and dopamine in neurochemical cell signaling.
Both ALS and Parkinson's disease have age related although the disease can appear at any age, it usually shows up after 20 and have a higher rate of occurrence after 50 to 60 years of age.
Could a person's ability to digest, absorb and/or repair fatty tissue slow down or become dysfunctional in relation to age? I guess it's like a 3 legged tripod stand, should any one of the legs in the tripod for healthy lipid-based membranes fail (digestion, absorption or repair) the entire system of having healthy fatty tissue might fail, unless there was some fail safe ability for humans to convert sugar to fat in humans.
Perhaps one treatment would be to exercise, which could raise the body's core temperature and temporarily restore the functionality of nerve tissue, (cycling helping patients with Parkinson's disease, a news story that broke in 2010)
http://www.medicalnewstoday.com/articles/253197.php
http://www.nytimes.com/2010/04/01/health/01parkinsons.html
http://www.foxnews.com/health/2012/04/24/bike-riding-helps-parkinsons-patients-ease-their-symptoms.html
So to reiterate, could Parkinson's disease (along with the main symptom of autonomous nervous system dysfunction) also be correlated with loss of thermoregulation?
Incidentally, another fatty tissue shows age correlation: the skin.
According to this website, 90% of people have age related sun spots by the time they are 60. This is something we can see all around us, people over 50 tend to have sun spots, and people close to 70 have a lot of large sun spots. https://zoskinhealth.com/blog/out-of-the-dark-reversing-sun-spots/
(and maybe there might be an entirely differently chemical co-factor I'm missing that is affecting phospholipid membrane permeability that is also age related).
I think that in studying the skin's sun spots (which thanks for the beauty industry, we have a lot of data on) it may be cheaper and quicker to draw parallels as to how rates of ALS and Parkinson's risk rate show up in relation to age as they are both fatty tissue type dysfunctions.
Oh dear I'm gradually turning into a theoretically biologist, as opposed to a real biologist.
found this later on
https://www.reddit.com/r/askscience/comments/1vfliv/how_do_deepsea_fishes_not_get_crushed_by_the/
Comments
Post a Comment